Hands on Lab Episode 3: Erler Zimmer 3D Printed Models
Nov 30th 2025
Anatomy Warehouse Webinar Episode 3: Erler Zimmer 3D Printed Models
Liz:
Hello and welcome to another episode of the Hands-on Lab here at Anatomy Warehouse. I am thrilled that you are joining us today because we've got a deeply fascinating session ahead, putting a spotlight on anatomical models that are leveling up how we teach human anatomy. In our last episode, we walked through Alex Gen AI from NASCO Healthcare, an AI-powered assistant simulation trainer pushing the limits of immersive education.
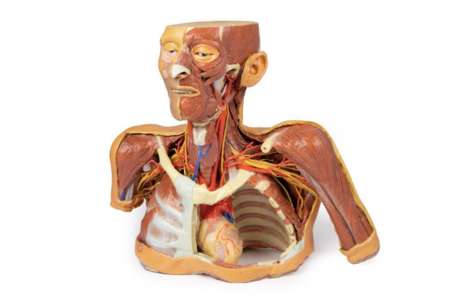
Today we're going to shift into another dimension of innovation, the Erler-Zimmer 3D Printed Anatomy Series. What sets these models apart is how they are made. Unlike traditional anatomical models, where they are molded and hand-painted, these models are brought to life by CT and MRI scans of actual human cadavers, and then using cutting edge 3D printing brought to life, like the ones you see here on the table.
Every vessel, every nerve, every muscle fiber is reproduced in natural color, with lots of depth, lots of detail. What you experience is anatomy with the intimacy and realism of a cadaver, but presented in a safer, more accessible, and reusable format. Today, we're going to have Anna and Mike, standing right over there, walk you guys through several signature models in detail, pointing out how their design solves for the challenges of working with cadavers, yet goes beyond standard anatomical models.
After that, we're going to have our guest speaker from Erler-Zimmer, whose name is Justin, share how the models are made with stories directly from the field. If you've ever wished you could bring a cadaver-style anatomy lab into your classroom, today's session is for you. Without further ado, Mike and Anna, welcome to the Hands-On Lab.
Mike:
Thanks, Liz. All right, so let's dive into the stars of today's episode, Erler-Zimmer's 3D printed anatomy series. These aren't just your average anatomy models.
They're created directly from real cadaver scans, capturing lifelike colors, textures, and anatomical accuracy right down to the smallest vessels and nerves. Each model tells a story, from vascular systems, nerve pathways, to real world pathology cases. Let's walk through some of our favorites.
Anna:
Absolutely, Mike, and we're starting with one of the most visually striking pieces, the 3D printed head, neck, and shoulder with angiosomes. This model combines multiple regions, the head, neck, upper chest, and shoulder, in one breathtaking lifelike dissection. On the right side, you'll see skin and superficial fascia intact with color-coded vascular territories, or angiosomes, mapped right onto the surface.
These zones represent real blood supply regions, critical for understanding surgical flaps, tissue viability, and reconstructive planning.
Mike:
Then on the left side, you get an entirely different perspective. The left side is fully dissected, exposing the muscle of the facial expression, mastication, and even deep structures of the infratemporal fossa. You can trace the common and internal carotid arteries and the internal jugular vein, and several cranial nerves, including the vagus and hypoglossal.
It even extends down into the axilla, where the brachial plexus roots and cords are visible. Along with the subclavian and axillary arteries, it's one of the few models that shows how the head, neck, and upper limb connect as one continuous anatomical system.
Anna:
Exactly. It's built for teaching. Students can see how the carotid sheath, clavicle, and brachial plexus interact.
You can trace the course of a nerve from the skull base all the way to the shoulder, making it a great tool for studying surgical anatomy, neurology, and physical therapy. And best of all, it's durable. Educators can handle this model year after year without losing any definition or color accuracy.
Mike:
Now let's take a look at another standout, the 3D-printed sagittal section of the head and neck. This model is like getting two in one. On one side, you've got a clean sagittal section showing the brain cavity, sinuses, and upper airway.
You can spot key structures like the dura mater, pituitary gland, and the cranial nerves as they pass through the skull. It really feels like opening a textbook, but in 3D. It's a textbook coming to life.
Anna:
Yeah. And when you rotate it, you get a completely new view. This lateral dissection opens up to the infratemporal fossa, revealing carotid arteries, jugular vein, and the vagus nerve.
You can also see the thyroid, larynx, and surrounding neck muscles all positioned exactly as they are in real life. It's detailed, accurate, and perfect for understanding how anatomical systems in the head and neck connect together.
Mike:
It's honestly one of the best head and neck teaching tools I've ever seen. This model is perfect for ENT, neurology, and surgical training because it bridges both the internal and external anatomy in one piece. And since it's based on real cadaveric dissection, you're seeing a true human variation, not a smoothed-out version of what...
not a smoothed-out version. It's what students will actually encounter in the field.
Anna:
So powerful. Alright. So let's take a look at something completely different.
Pathology in 3D. This is a 3D-printed melangioma model, part of Ehrler-Zimmer's pathology series. It's based on a real patient specimen featuring a six-centimeter melangioma between the two frontal lobes.
You can see the tumor here. It's that pinkish-yellowish mass nestled right between the two frontal lobes, compressing them on both sides. It's an incredible visual.
And what makes this even more remarkable is that you're not just looking at a diagram. You're seeing a real-life clinical case faithfully recreated in 3D from actual patient data. Getting to hold a model like this and explore it up close and tracing the anatomy surrounding the tumor is an experience that very few people will get outside of a surgical or pathology lab.
And like all models in the pathology series, this one includes an authentic clinical history of the patient it was replicated from. That means that every model tells its own story, connecting what you see in the anatomy to what happened in real life.
Mike:
This one really bridges the gap between anatomy and clinical medicine. Instead of just showing where a tumor might be on a diagram, students can hold an actual 3D representation. That's huge.
See how it displaces structures, understand the spatial relationships, and connect symptoms to anatomy. It's perfect for neurology, pathology, and radiology programs because it brings textbook cases to life in a tangible way.
Anna:
Yeah, exactly. And that's what makes this whole 3D printed model series so powerful. You're not just teaching anatomy.
You're teaching real human anatomy. You're showing students what structures look like, how they relate, and how they can change in disease. The angiosomes model teaches us living vascular mapping.
The sagittal head and neck model bridges clinical and structural learning. And the melanchoma model brings pathology right into any classroom or lab. Together, models from this series create a complete hands-on understanding of human anatomy in context.
Mike:
Well said, Anna. These models make anatomy accessible, accurate, and consistent. No lab chemicals, no short specimen lifespans, just pure repeatable learning.
Whether it's a med school, a nursing program, or surgical residency, this is how modern anatomy education looks. Let's keep things moving. So we'll dive into how educators are using these in the classroom and what kind of results they're seeing.
So now that we've had a close-up look at the models, let's talk about how they're used in classroom and labs. These 3D printed anatomy models aren't just display pieces. They're practical teaching tools designed for hands-on learning.
Liz:
Exactly. And they really shine in medical and nursing education. In programs that don't typically have cadaver labs, these models become essential.
Students will get a real tactile visual learning experience tracing every nerve, vessel, and muscle with their own hands. For example, this agital head and neck model lets students study structures like the pituitary gland and the carotid arteries and the cranial nerves in precise 3D orientation. It bridges the gap between textbook learning and actual spatial understanding.
Mike:
That's such a good point, Anna. And for educators, they're a game changer for small group instruction. Instead of five students crowding around a single cadaver, each group can have their own model and every one of them is exactly the same.
You can pass around a brain model, a vascular limb model, and know that every student is getting the same view, the same details, and the same opportunity to learn.
Liz:
And that consistency is huge. Take the head, neck, and shoulder with angiosomes model, for example. It's perfect for teaching vascular territories, how blood supply zones interact across the face, neck, and shoulders.
Students in reconstructive surgical programs can literally plan flat procedures on this model, tracing where arteries flow and where tissue viability changes. That's a level of interaction that's nearly impossible with static images.
Mike:
And when it comes to pathology and clinical training, these models are just as powerful. The meningioma model is one of my favorites because it takes a real patient case and puts it directly into the student's hands. They can see how the tumor compresses the frontal lobes and how it distorts surrounding tissue.
And what that means for neurological function, you're not just reading about pathology, you're seeing it, you're holding it and understanding its impact on real anatomy.
Anna:
Yeah. And it's not just for students either. Clinicians can use these models to explain complex conditions to their patients, showing them exactly what's happening inside of their bodies.
Surgeons can use them for preoperative planning, especially with vascular and cranial procedures. They can map pathways, visualize challenges, and prepare before ever entering the OR.
Mike:
It's also worth mentioning how much these models help with knowledge retention. Instructors we've talked to say their students come into cadaver labs or clinical rotations far more prepared. They've already memorized where the vessels are located, nerve pathways, and even the spatial relationships.
They can just focus on technique rather than the orientation. One professor even said her students' test scores jumped after introducing 3D printed models into her curriculum.
Liz:
That doesn't surprise me at all. And beyond education, there's a real long-term investment for institutions. There's no special ventilation, no chemicals, no preservation costs or ethical concerns.
Once you have these models, they last for years. No degradation, no fading. You just wipe them down and they're good to go for the next use, ready to go right outside the box.
Mike:
Exactly. And that's because they're printed from real cadavers. Every model reflects natural variation of human anatomy.
Students aren't looking at a perfect version. They're seeing real-world differences, asymmetries, branching patterns. That's the kind of authenticity that helps bridge the gap between study and practice.
Anna:
So whether it's medical schools, nursing programs, or surgical training centers, these 3D printed models deliver a learning experience that's accurate, repeatable, and visually stunning. They make anatomy accessible without losing the realism of the real human body.
Mike:
It's hands-on learning without the barriers of traditional cadaver training. And that's exactly what makes them so effective. So now what we'll have is Justin Adams from Monash University.
We'll be speaking about the process of creating these models and the unique benefits of using these products in the classroom.
Justin:
Hi, my name is Justin W. Adams, and I'm an associate professor and I'm the current director of the 3D Innovation and Design Studio at Monash University. As one of the original creators, it's a pleasure to have the opportunity to answer some of the questions we've received about the 3D print series that we've developed.
I will talk to most of those questions. The one question I will not answer, though, is which is my favorite 3D print, because I'm not going to pick and choose amongst all the children that we've developed over the last 11 to 12 years. So with that said, I'm going to turn to some answers, and hopefully this will provide you greater insight as to the work that we've done, how we've achieved this, and maybe a few glances at some of the future directions.
Monash University, based in our Clayton campus in Melbourne, engages nearly 2,000 students a year in some type of anatomy instruction. This ranges from undergraduate and graduate entry medical courses through to biomedical and developmental biology units, allied health courses that cover the spectrum from physiotherapy to the radiological sciences. In short, we're very busy people, and this created a clear problem for us as we looked to future-proof our strategy for how anatomy education would take place in the future, particularly as we transitioned into brand new teaching facilities that we really moved into just a few years ago.
We wanted to consider a range of different approaches, both those traditional and potentially cutting-edge, so that when we moved into these facilities, we'd be able to engage our students in the fullest possible way. As academics, we prioritize publishing the details of our methodologies. Our first paper in 2014 outlined the steps we employed for using commercially available hardware and software to turn anatomical specimens into 3D prints.
In 2024, we followed up on our original publication to provide further technical details on how our process has adapted over time in response to changing technologies in the space. In brief, we begin with a carefully dissected specimen that is digitized, either using a standard medical computerized tomography scanner to achieve a high-quality reconstruction of the sectional anatomy, or use of a full-color handheld surface scanner. Once the original specimen has been digitized, we produce a 3D mesh file through careful editing and adjustment to achieve the final design.
Depending on the goal for the final print appearance and use in a classroom, we then edit and adjust color and any key adjustments needed to produce a printable file. While over the past 12 years our methods have evolved and refined as the technology around 3D data capture and printing has changed, and is reflected in our publications on this, the general approach has been used for all three of our currently available anatomy replica series. First series, Series 1, consists of 60 anatomy replicas that were designed by us to cover all body regions and different levels of dissection.
Our prints are based on donor tissue that had been professionally dissected and have been digitized using high-resolution computerized tomography. We selected a range of specimens that would address core anatomy curriculum across a whole series of units and levels of instruction, with our use of false color allowing us to maximize the approachability of these replicas across a diverse range of undergraduate and graduate anatomy units, as well as within the basic sciences and allied health fields. We've been adapting our first series of anatomy models for production on new generations of UV curable resin printers.
These printers allow us not only richer color reproduction, but the ability to integrate clear supports and additional shells in order to enhance model durability, particularly with handling in classroom environments. This new generation of 3D printers also allows us to capture and harness photorealism, particularly from changing technologies within 3D data capture. Our second series, Series 1.1, was designed to complement and expand our first series. This was released for 2021 with 59 new 3D prints. Our Series 1.1 prints blend different high-resolution digital data capture methods from computerized tomography through to full color 3D scanning. Our 3D prints in the series provide a mix of realistic donor tissue colors with false color overlays for key anatomical structures, and truly expands on our original series to include individual organs, complex anatomical regions like the thorax, abdomen, pelvis, and the head and neck.
And also released in 2021 is our Series 2, which represents our first range of replicas of pathological anatomical conditions. A true rarity in current teaching collections and traditionally only viewed by students in historical pots, we have used our photorealistic capture methods to reproduce a range of 88 pathology replicas from across major organ systems. These provide a truly unique opportunity to integrate physical replicas into the teaching of human pathology and disease, ranging from neurological tumors and polycystic kidney disease through to tuberculosis and advanced stage cancer.
There are several different ways that a new 3D print will come into existence. Generally, we start from an identified need within a course. This can be a region that isn't yet represented in our catalog or a request to generate a new model because curriculum changes have created a demand for a new teaching tool.
We will develop a prospectus of what the replica is meant to provide and then identify either an existing donor tissue prosection within our teaching collections or develop a new dissection. For example, recently one of our staff highlighted a need for more 3D prints that include back anatomy, ideally including several layers of musculature, particularly between the back and the neck regions. In this case, we are able to take advantage of an existing prosection in our teaching collection, but realized we would have to be creative in producing a teaching model that would capture multiple layers within a single print.
Using surface scanning, we acquire the primary dataset and then generate an initial 3D file to begin cleaning, hole filling, and editing. In this case, as only the back was essential, we effectively skip scanning the rest of the body. More on that in a minute.
This production of an early draft of the model allows us to fact check the reconstructed 3D surface against the original specimen. This process can go through several rounds of checking and editing of the digital file in reference to the prosection, ensuring that there has been accurate capture of the details of the anatomy. We also consider any mechanical production issues, including where we believe structures will require supports or creative solutions to translate the specimen into a printable object.
In this case, we scanned the original prosection in two different positions of muscle layers and then created a false geometry base, as we hadn't bothered capturing data from the entire specimen. This allowed us to be both creative and cost effective, using a common base that provides structural reference points for teaching, but different superficial and deep insert layers that would allow staff to swap during teaching and expand the use of the print. Now, once we have the geometry of the model completed, we move on to color management, again, working back and forth with the original specimen and our staff to generate any artificial changes to reach the, quote, teaching version.
We then generally print one or two prototypes to confirm the reproduction of both the color and geometry in the 3D print. This allows us to do a final check of the 3D print against the original before final edits and adjustments and finalization of the print file. There are several key ways in which our 3D prints vary from traditional anatomy models and contribute to their impact in educational environments.
One of these ways is that our prints are effectively one-to-one reproductions of actual human anatomy as opposed to sculptural representations. This means that the size of anatomical structures like blood vessels, lymph nodes, nerves, and the proportional and spatial relationships of structures reflect their actual condition. We've also captured the true complexity of anatomical structures, including diverse branches of blood vessels and nerves that are regularly simplified or absent in traditional anatomy models.
We've also used 3D manufacturing methods where we're able to represent anatomical relationships that are freed from the limits of traditional molding and casting. This means our anatomy replicas have undercuts, freestanding structures, and other model design features that are effectively impossible to produce in traditional models. Another benefit is that we've developed a true range of anatomy replicas that demonstrate the same anatomical structures from different perspectives, sections, or levels of dissection.
This diversity means that not only do we have more than just a head and neck replica or a knee joint, but we also have captured levels of individual variation in the sizes of structures and in configurations anatomically that afford diverse teaching and assessment opportunities. A second obvious benefit is that our 3D replicas allow us to work with multiple copies of identical anatomy across the classroom. We don't have to have students crowded around a single specimen.
We can distribute identical copies of anatomical specimens and structures across multiple classrooms, student groups, or environments so that everyone has equal access to the same information. Another benefit is that we've chosen to amplify some of these anatomical structures to aid in teaching. One obvious example of this that I've already talked about has been our selection of false colors or true color overlays in order to enhance certain anatomical structures and to make them stand out.
But there are other ways that we've taken advantage of 3D printing by changing the scale of some structures in order to make them easier to demonstrate, like very small structures, inner ear anatomy for example, and using digital data tools to demonstrate relationships that can be very difficult to see in real human tissue. First off, we find that our 3D prints are a really great and effective tool for students to transition from textbook illustrations and introductory content into understanding really complex regions of anatomy, particularly where in donated and preserved human tissues, structures like nerves, blood vessels, arteries, and veins, particularly in tight and compact anatomy regions like the orbit, are all going to look the same. The second thing is that we use our 3D prints when we're undertaking dissection-based teaching because they provide a very useful tool for displaying goals in dissection sections, essentially a preview of the anatomy that they should expect to see when moving through layers and understanding the courses of structures that are still hidden by layers of tissue that have not yet been removed.
Our prints are obviously very durable and are an inorganic material, which as I've mentioned means that we can move them around lab settings in different lab environments, so we can move them into spaces to help demonstrate and reinforce content even if the objective of that session isn't as a practical. That transportability across teaching spaces is really just something that we can't do with wet tissue specimens, particularly given the logistics of working with donor tissue. And our prints make a really excellent assessment tool, particularly because you can plan the structures that you want to test student knowledge on well in advance, and you'll be confident that those structures will be present when you want to assess students on their understanding of anatomical regions.
As an anatomy educator with nearly 25 years worth of experience, I'm fortunate enough to be able to speak to both the feedback we've received directly from students and other staff members working with our 3D printed anatomy replicas across a variety of units, but also to the overall benefits that we've seen using our 3D prints in our classrooms over the past decade. Over the years of working with 3D prints in anatomy teaching, we've seen a number of real tangible positive benefits for our students. These are things that we actually summarized and put together within a peer-reviewed paper a number of years ago within the journal Anatomical Sciences Education, and we've seen spur a large body of academic research into the impacts of 3D prints, replicas, simulators within anatomy education environments.
The first thing that we've seen is probably one of the biggest impacts is in their approachability, particularly for first-year medical students, students in the sciences, and students in allied health fields. Donor tissues can be challenging and confronting for some students, and they are preserved in chemicals, they can evoke all sorts of reactions to younger students, particularly when they're presented in varying states of dissection. They can be difficult to move, heavy, hard to manipulate.
So for all these reasons, we oftentimes encounter hesitancy by students, sometimes avoidance of working with donor tissues, particularly with direct handling early on in their education. As an inorganic alternative, however, our 3D prints have the rich detail that students need, but also provide them with the confidence to be able to pick up what they don't view as being human tissue. They don't have to necessarily use gloves, deal with chemicals, they don't have to deal with wet tissues or the knowledge that they are directly handling human remains.
We see them picking up our 3D prints, we see them rotating them in their hands, getting close, investigating the anatomy with confidence, and all without having lost any of the critical detail and fidelity of actual human anatomy. So it's for these reasons amongst others that we've already discussed today that we see real tangible benefits for our students using 3D prints, particularly in outcomes of anatomy learning. We've seen statistical evidence indicating that students who do use our 3D resources in classrooms do better in assessments or gain confidence more quickly with understanding anatomical structures than just when using either traditional models or just cadaver-based instruction.
Mike:
Thanks again, Justin, for joining us and for giving us that incredible insight with behind the scenes of how the 3D printed anatomy series came about. It was incredible to see how these amazing products came to be and now let's get into a Q&A section of the episode. If you have any questions, be sure to drop them in the chat.
For now, we have a couple questions prepared. Let's get into them now.
Anna:
Sounds good, Mike. So how durable are these models when you compare them to real cadavers?
Mike:
So the benefit of these models is that they are reusable, cleanable, and they allow multiple uses without having to discard the model or the cadaver afterward. So while still having some fragile parts of the model, such as the nerves and the arteries, this model is built to handle sustainable usage in the lab. And really what it does is it helps you practice handling a cadaver.
So, you know, with care.
Anna:
So how could I purchase one of these anatomy models?
Mike:
We could all purchase these by going on our website, anatomywarehouse.com. We have a section in our menu under anatomy models called 3D printed models. That's where you'll find all the models, veterinarian, human, you know, all the sorts.
Anna:
Okay final Question – what types of models are covered?
Mike:
We offer are a wide breadth of healthy and pathology models as well as veterinary models of a selection of animals. I know we have a dog head where you can see different layers like skin within a dog. With almost 200 models available, we can help set you up with the perfect model you are looking for.
Anna:
Sounds extensive! Alright, so were going to hand it back off to Liz for our outro today, Liz, come on back!
Liz:
Great job, Mike and Anna, you guys really dissected today’s presentation!
It’s been awesome to showcase the 3D Anatomy Series, it’s a personal favorite of mine in our product lineup. A big thank you to Justin from Erler Zimmer for joining us, and thanks to all of you for being here today.
Don’t forget to check out the full lineup of 3D Printed Cadaver Replicas on AnatomyWarehouse.com, the only place you can order these in North America.
As always, our team is here to help you pick the right models for your anatomy lab, so reach out any time by phone, email or, even better, visit us right here in our showroom!
Before I go, a quick teaser: in our next episode, we’ll be exploring the new SAM4 Adult Auscultation Manikin from 3B Scientific. Tim from 3B will join us and you won’t want to miss it.
And with that, this will wrap up today’s episode of the Hands-On Lab. Until next time, stay curious, stay engaged, and as always, stay hands-on!
FAQ
How durable are these models when you compare them to real cadavers?
The benefit of these models is that they are reusable and cleanable – allowing multiple uses without having to discard of the model after initial use. While still having some fragile parts of the model such as nerves and arteries, this model is built to handle sustained usage in the lab.
How could I purchase one of these anatomy models?
Visit Anatomywarehouse.com and find the 3D printed models on the menu bar to view our entire lineup of 3D printed Anatomy Series Models.
What types of models are available in the 3D printed Anatomy Series Models?
We offer are a wide breadth of healthy and pathology models as well as veterinary models of a selection of animals. With almost 200 models available, we can help set you up with the perfect model you are looking for.
How durable are these models when you compare them to real cadavers?
The benefit of these models is that they are reusable and cleanable – allowing multiple uses without having to discard of the model after initial use. While still having some fragile parts of the model such as nerves and arteries, this model is built to handle sustained usage in the lab.
How could I purchase one of these anatomy models?
Visit Anatomywarehouse.com and find the 3D printed models on the menu bar to view our entire lineup of 3D printed Anatomy Series Models.
What types of models are available in the 3D printed Anatomy Series Models?
We offer are a wide breadth of healthy and pathology models as well as veterinary models of a selection of animals. With almost 200 models available, we can help set you up with the perfect model you are looking for.
Why are 3D printed anatomical models considered more advanced than standard teaching models?
Because the manufacturing process uses multi-material 3D printing and true anatomical data, these models show real color differentiation and physical structures that mimic actual human specimens. Unlike traditional models, which are stylized or simplified, these prints offer near-cadaveric fidelity without ethical or logistical barriers.
Because the manufacturing process uses multi-material 3D printing and true anatomical data, these models show real color differentiation and physical structures that mimic actual human specimens. Unlike traditional models, which are stylized or simplified, these prints offer near-cadaveric fidelity without ethical or logistical barriers.
Do these 3D printed anatomy models require special handling like cadaveric specimens?
No because the models are printed replicas and not actual biological tissue, they avoid safety, ethical, regulatory, and storage issues associated with preserved specimens. Educators can use them freely in classrooms and labs without the restrictions that come with real cadavers.
No because the models are printed replicas and not actual biological tissue, they avoid safety, ethical, regulatory, and storage issues associated with preserved specimens. Educators can use them freely in classrooms and labs without the restrictions that come with real cadavers.
How can educators integrate these models into teaching curricula?
The models can be used for lectures, lab demonstrations, student workstations, and clinical case discussions. Their anatomical accuracy makes them ideal for foundational learning and advanced study, helping programs create modular learning stations and hands-on student exploration of complex structures.
The models can be used for lectures, lab demonstrations, student workstations, and clinical case discussions. Their anatomical accuracy makes them ideal for foundational learning and advanced study, helping programs create modular learning stations and hands-on student exploration of complex structures.
Share: